The international development, led by Tel Aviv and Harvard universities, may significantly optimize the process used today in drug development, and save time, resources and suffering involved in animal experiments and human clinical trials. Two articles on the subject were published in the journal Nature Biomedical Engineering

Researchers from Tel Aviv University succeeded in developing an innovative system that connects several organs-on-a-chip, and simulates the operation of entire systems in the human body. The innovative method may bring about a real revolution in the process of drug development - which currently takes many years and costs a lot of money, and despite this is only partially effective. Another possible advantage of the new technology is the prevention of the ethical problems associated with animal experiments.
The studies were carried out in collaboration with Harvard University, with the participation of 57 researchers from research institutions and drug development companies around the world. Both articles were published in the journal Nature Biomedical Engineering in January 2020.
"Drug development today involves a process that takes 20-10 years, and costs about 2-1 billion dollars per drug," explains Dr. Ben Maoz from the Department of Biomedical Engineering and the Sagol School of Neuroscience at Tel Aviv University, who is one of the leaders of the international project. "Out of it, about 6-3 years are dedicated to experiments on cultures and animals, and another 8-6 years are dedicated to clinical experiments on humans. And after all the effort and investment, it turns out that the process is ineffective: about 90-60% of the drugs that benefit animals fail in humans. This situation causes researchers all over the world to look for alternative procedures for drug development. One of the technologies with the greatest potential in the field is OOC (Organ-on-a-Chip), or in Hebrew 'organ-on-a-chip.' As part of the method, which was first developed in 2010 at Harvard University, the scientists use cells from a certain human organ - heart, brain, kidney, lungs, etc., and with the help of tissue engineering techniques, place them in a plastic cartridge - otherwise known as the chip.
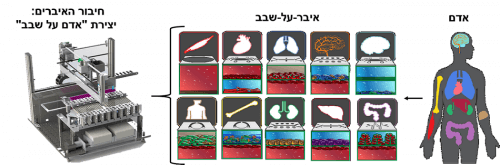
In recent years, a wide variety of 'organs-on-a-chip' has been developed in the world that function like the human organ itself. About two years ago, Dr. Maoz developed an organ-on-a-chip that mimics the action of the blood-brain barrier, and in other places chips for the heart, kidneys, intestines and more have been developed. In the current project, a system was developed for the first time that is able to connect the various chips, and allows simulating the operation of entire systems in the human body, and their response to experimental drugs that are fed into the system.
The system was developed and tested in two studies: in the first study, the researchers developed an automatic robotic system that can connect in a simple and modular way between chips of up to 10 different organs, and allows control of any material that enters and leaves each chip. In addition, they created a suitable and supportive biological environment for the tissues on the chips, a sort of 'artificial blood', which allows them to function and communicate with each other over time. The researchers placed 9 organs-on-a-chip in the system - brain, blood-brain barrier, lungs, heart, bone marrow, kidney, intestine, liver and skin, and found that it works successfully for at least three weeks.
In the second study, the researchers added different drugs to the automatic system, and tested how the different organs reacted. First, nicotine was introduced into the system, a substance that is usually taken orally to help quit smoking, and is currently also being tested as a medicine for degenerative diseases and chronic inflammation of the intestine. "For drugs that are taken orally, the absorption process of the drug in the body is of great importance - through the intestine that absorbs it, the liver that breaks it down and finally the kidney that filters the substance," says Dr. Maoz. "Therefore, for nicotine, we placed in our platform chips of these three organs." The second drug tested was cisplatin, a common ingredient in intravenous cancer chemotherapy treatments. For her, liver and kidney chips were placed in the system, as well as a bone marrow chip - which is greatly affected by the drug.
The next challenge was to adapt the results measured on the innovative platform to the human body as a total system, and to bridge the gaps between them. To this end, the researchers developed computational models that translate the values obtained in the system into parallel results of clinical tests in humans. Indeed, the combination between the automated organ-on-a-chip system and the computational models produced values very close to those measured in human patients in the clinic.
"For the first time in the world, we were able to develop a reliable and flexible organ-on-a-chip platform, which gives results very close to those obtained in human patients," concludes Dr. Maoz. "Already today, after the American Drug Administration (FDA) announced that it supports the development of organs-on-a-chip that will be used as a supporting tool for drug development, companies and laboratories working in the field can use our system. We also believe and hope that in the future, after further development, the new platform can be used as an alternative to animal experiments and even to a considerable part of human clinical experiments. In this way, it will save years of research, a lot of money, and the suffering of both humans and animals."
