The printed glioblastoma tumor, the deadliest type of brain cancer tumor, is printed from human tissue and contains all the components of the cancerous tumor * The researchers estimate that in the future it will be possible to quickly predict the most suitable treatment for the patient and at the same time develop new drugs at a much faster pace than what exists today

A scientific achievement for researchers from Tel Aviv University who managed to print a complete and active glioblastoma cancerous tumor with a XNUMXD printer. The printed tumor includes a branched system of blood vessel-like tubes through which blood cells and drugs can be flowed in a manner that simulates the real tumor.
The research was conducted under the leadership of Prof. Ronit Sachi-Painero From the Sackler Faculty of Medicine and the Segol School of Neuroscience, who heads the Cancer Biology Research Center, the Cancer and Nanomedicine Research Laboratory, and the Morris Kahn XNUMXD Cancer Research Project at Tel Aviv University. The new technology was developed by doctoral student Lena Neufeld along with laboratory members Elam Yeni, Naa Reisman, Yael Shtilerman, Dr. Dekala Ben-Shoshan, Sabina Pozzi, Dr. Galia Tiram, Dr. Anat Alder-Bock, and Dr. Shiran Farber.
The tumor printing is based on patient samples taken directly from the operating rooms in the neurosurgery department at Sourasky Hospital in Tel Aviv. The results of the new study are published today in the prestigious journal Science Advances.
"Glioblastoma is the deadliest type of cancer in the central nervous system, and it constitutes the majority of malignant tumors originating in the brain," says Prof. Sacchi-Painero. "In our previous research, we identified for the first time a protein called P-Selectin, which is secreted at the meeting between cancer cells of the glioblastoma type and cells of the microglia type, the cells of the immune system in our brain. We found that this protein is responsible for the failure of the microglial cells which, instead of attacking the cancer cells, encourage the spread of this deadly cancer. But we detected this protein in tumors surgically removed from patients - but not in glioblastoma cells that we grew in my laboratory, in two dimensions on petri dishes. The reason is that cancer, like any tissue, behaves very differently on a hard plastic surface compared to its behavior when growing in the human body. 90% of the drugs fail at the stage of clinical trials because they fail to reproduce in humans the success achieved in the laboratory."
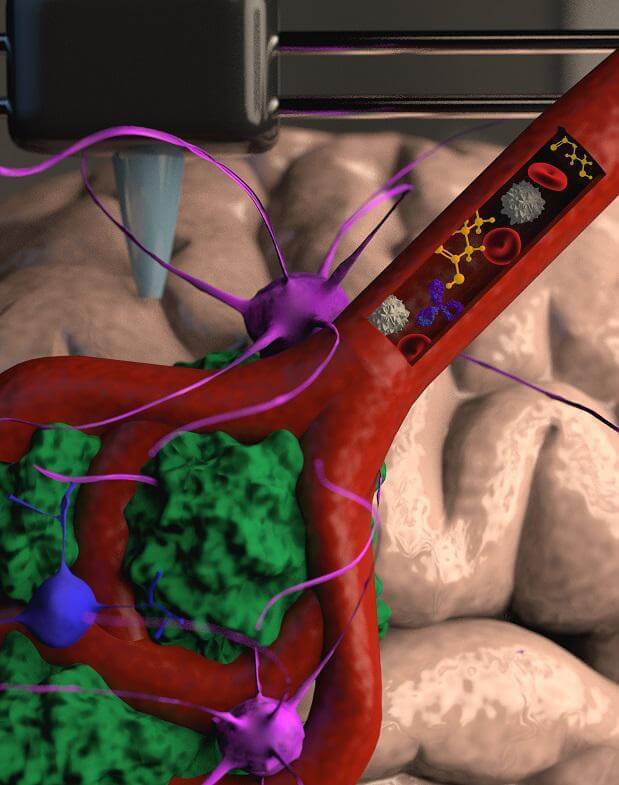
To this end, the team of researchers led by Prof. Sachi-Painero together with doctoral student Lena Neufeld, winner of the prestigious Dan David scholarship, created the first XNUMXD printed model of a glioblastoma type of cancer that includes XNUMXD cancerous tissue, surrounded by an extracellular matrix and communicating with its environment through functioning and flowing blood vessels.
"It's not just the cancer cells themselves," explains Prof. Sachi-Painero, "but also the cells of the microenvironment in the brain, the astrocytes, microglia and blood vessels connected to a microfluidic system - that is, a system that allows substances such as blood cells and drugs to be injected into the tumor. Each model is printed in a bioreactor that we produced in the laboratory, using a gel that we modeled and replicated from the extracellular matrix taken from the patient, thereby simulating the tissue itself. After all, the brain does not have the same physical and mechanical properties of other organs such as skin, breast or bone. Breast tissue is mostly fat, bone tissue is mostly calcium; Each tissue has different properties, and these properties affect the behavior of cancer cells and their ability to respond to drugs. Growing all types of cancer on the same plastic surface is far from optimally simulating the clinical situation."
After successfully printing the XNUMXD tumor, Prof. Sachi-Painero And her colleagues showed that with the help of the model, it will be possible to quickly and efficiently predict the most suitable treatment for a specific patient, in contrast to cancer cells growing in petri dishes.
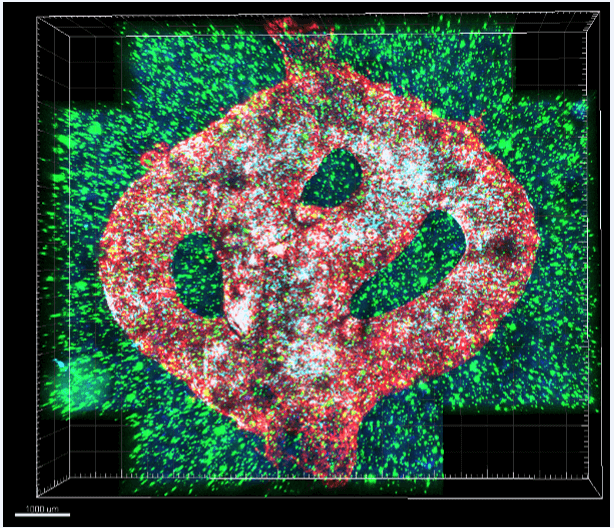
"We proved that our XNUMXD model is more suitable for predicting and developing drugs in three different ways. First, we tested a substance that inhibited the protein we found, P-Selectin, on glioblastoma cell cultures in two-dimensional Petri dishes, and we did not see any change in the division or migration of the treated cells compared to the untreated control cells. On the other hand, in model animals and in the XNUMXD printed models, where we did find a high expression of the protein, we were able to delay the progression of the glioblastoma by blocking the P-Selectin protein. This experiment proved to us how many potential drugs do not reach the clinic because they failed tests on two-dimensional models, and vice versa: some cases that were considered a resounding success in the laboratory, failed the clinical tests.
In addition, in collaboration with the laboratory of Dr. Assaf Medi from the Department of Pathology at the Faculty of Medicine at Tel Aviv University, we genetically sequenced the cancer cells that we grew in the XNUMXD model and compared them to cancer cells that grew on XNUMXD plastic and cells that we sequenced from patients, and showed that the XNUMXD printed tumors were much more similar to brain cancer cells in their natural environment. Over time, the cancer cells grown on plastic gradually changed until they lost all connection to the cancer cells in the patient's brain. Finally, the third proof was by measuring the growth rate of the crops. Glioblastoma is a violent disease, among other things, because it is unpredictable: if the heterogeneous cancer cells are injected separately into model animals, in some of them, the tumor will be dormant and in some, an active tumor will quickly develop. This makes a lot of sense because we humans can die in good health without even knowing that we had such 'dormant' tumors. In contrast, on the plastic plate in the laboratory, all tumors grow at the same rate and spread in the same manner. In the tumor we printed with the XNUMXD printer, the growth rate of the tumor corresponds to the development we see in patients or model animals."

According to Prof. Sacchi-Painero, this is an innovative approach that will allow both the development of new drugs as well as the discovery of new targets for suitable drugs at a much faster rate than what exists today. In the hope that in the future, this technology will enable personalized medicine for patients.
"If I take a sample from a patient's tissue, along with its extracellular matrix, I can print a hundred different tumors from this sample and test many drugs and in different combinations to find out which drug or combination of drugs is more suitable for this specific tumor. Alternatively, the development allows us to test a lot of different compounds on a tumor printed with a XNUMXD printer, and decide which compound is worth investing the resources in to try and develop further as a medicine up to the clinical stage. But perhaps the most exciting part is finding the target proteins and target genes in the cancer cells, something that is very difficult to do in tumors found in the brains of patients or animal models. The innovative development gives us unprecedented access, and not limited in time, to examine in depth a XNUMXD tumor that mimics the tumor we find in the patients in the best possible way."
The study was funded by the Morris Kahn Foundation, the Israel Cancer Research Fund (ICRF), the European Research Council (ERC), the Cancer Society, the National Science Foundation and Check Point Software Technologies Ltd.
More of the topic in Hayadan:
- A new immunotherapy helps the cells of the immune system locate the deadly glioblastoma brain cancer cells and eliminate them
- Activating the brain's immune system against the deadly glioblastoma cancer makes it possible to stop its spread
- Researchers at the Hebrew University have discovered new markers for diagnosing the severity of brain cancer and a new way to treat the disease
- Against four cells - why is there currently no effective drug for the treatment of glioblastoma brain cancer?

One response
Important information is missing
How do you actually print the tumor on the printer? With what materials? Or perhaps only the outer skeleton of the tissues is printed and then the tumor is allowed to develop a child with the healthy tissues on its own?